Why Spinal Tumour Surgery Can Cause Serious Blood Loss and How UAE Surgeons Manage It
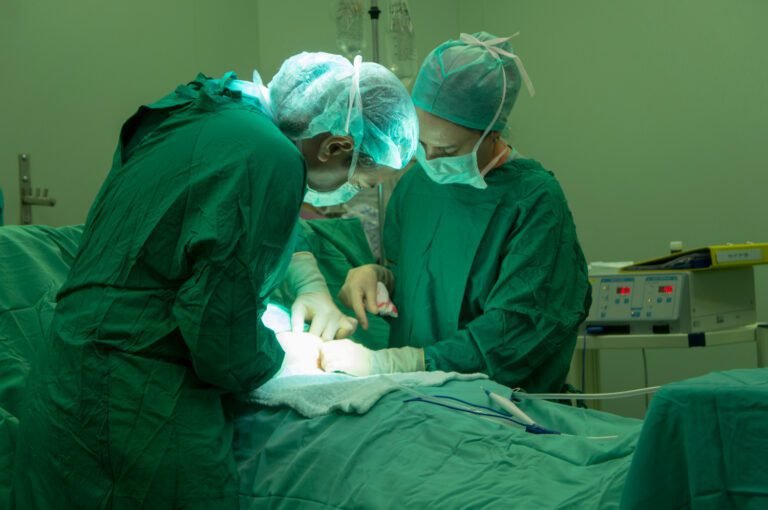
Is spinal tumour surgery always high risk for blood loss?
Not always. The risk depends on the tumour type and its vascularity. Simple intradural tumours such as schwannomas often involve very modest blood loss. Highly vascular metastases from kidney or thyroid cancers carry a much higher haemorrhagic risk and require specific pre-operative preparation.
What is the recovery like after spinal tumour surgery?
Recovery varies significantly depending on the extent of the surgery, the patient’s neurological status before the operation, and their overall health and oncological situation. Simple decompression procedures may allow mobilisation within a day or two. Extensive reconstructive procedures with long fusions require longer recovery. Oncology treatment including radiotherapy or systemic therapy typically continues after surgical recovery.
Can all spinal tumours be surgically removed?
No. Surgical removal is appropriate for certain tumour types and in certain clinical situations. For many patients with spinal metastases, surgery is focused on decompression and stabilisation rather than complete removal. Some tumours are not safely resectable due to their proximity to the spinal cord or major vessels. Treatment decisions are made on a case-by-case basis by the multidisciplinary team.
What is the difference between radiotherapy and surgery for spinal tumours?
Radiotherapy can control certain tumour types without surgical intervention and is used before surgery (to reduce tumour size), after surgery (to treat residual disease), or as the primary treatment when surgery is not appropriate. Surgery is needed when there is acute neurological compromise, spinal instability, or when tissue is needed for diagnosis. Most patients receive a combination of both.
How is embolisation performed and is it safe?
Embolisation is performed by an interventional radiologist under X-ray guidance, usually under sedation. A catheter is introduced through a small puncture in the groin and guided to the vessels feeding the tumour. Embolic material is then injected to occlude these vessels. It is generally a safe procedure when performed by an experienced team, with the main risks including inadvertent embolisation of adjacent vessels and post-procedure pain as the tumour loses its blood supply.
Should I seek a second opinion before spinal tumour surgery?
For any significant surgical procedure involving a spinal tumour, a second opinion from a specialist spinal oncology team is entirely appropriate and should be welcomed. The complexity of these cases means that multidisciplinary input, including oncology, radiology, and surgery, is standard practice in specialist centres.
Spinal surgery covers a wide spectrum of procedures, from a microdiscectomy that takes under an hour and involves minimal blood loss, to complex tumour resections that can test the limits of what surgical teams can safely manage. The difference in blood loss between these two extremes is not incidental. It reflects fundamental differences in the biology and vascularity of the pathologies being treated, and understanding this difference explains why spinal tumour surgery requires a level of preparation and expertise that goes far beyond standard decompression or disc surgery.
Dr. Sherief Elsayed, Consultant Spine Surgeon in Dubai, explains the challenge directly and describes the specific strategies used to manage it.
How Much Blood Loss Is Normal in Spine Surgery?
Blood loss is an unavoidable aspect of surgery, but the amount varies enormously depending on the procedure.
Dr. Sherief Elsayed contextualises this with a clear comparison: “I lose 10 to 100 mils of blood if I’m doing a simple discectomy or a decompression, for example. If, on the other hand, I’m doing a tumour, I could lose two litres of blood, especially if it’s a very vascular tumour.”
To put those numbers in perspective, an adult human body contains approximately 4.5 to 5.5 litres of blood. A blood loss of 10 to 100 millilitres during a microdiscectomy is clinically insignificant. A blood loss of two litres, representing approximately 40 percent of the total blood volume, is a major haemorrhagic event requiring careful management and often blood transfusion. The surgical team, the anaesthetic team, and the theatre setup must all be prepared for this possibility before incision.
Why Do Tumours Bleed So Much?
The answer lies in tumour biology, specifically in the way tumours develop their own blood supply.
Malignant tumours that spread to the spine (metastatic tumours) arrive there via the bloodstream. The spine’s abundant venous plexus, particularly in the vertebral bodies, makes it one of the most common sites for metastatic disease. When tumour cells establish themselves in the vertebral bone, they stimulate the formation of new blood vessels to feed their growth. This process, called angiogenesis, produces a network of abnormal, thin-walled, fragile blood vessels that are far more prone to bleeding than normal tissue.
Certain tumours are particularly vascular, as Dr. Sherief Elsayed notes: “Kidney cancers or thyroid cancers that are spread to the spine, they’re very, very vascular and they bleed a lot.”
Renal cell carcinoma (kidney cancer) is notoriously hypervascular. Its metastases to the spine can bleed catastrophically when incised without preparation. Thyroid cancer metastases share this characteristic. Hepatocellular carcinoma (liver cancer) is another highly vascular tumour that frequently metastasises to the spine and presents the same haemorrhagic challenge. In contrast, metastases from lung or breast cancer, while common, tend to be less vascular and more manageable from a bleeding standpoint.
What Is Embolisation and How Does It Reduce Blood Loss?
The most important pre-operative strategy for managing vascular spinal tumours is embolisation, a procedure performed by an interventional radiologist before the surgical team operates.
Dr. Sherief Elsayed describes the process: “If we can, we try and embolise those very vascular tumours before we operate. I ask one of my radiology colleagues to feed a catheter to the feeding vessel of the tumour and then inject some stuff which essentially cuts off its blood supply. That can help reduce blood loss during surgery.”
How embolisation works:
A thin flexible catheter is introduced through a small puncture in the groin and guided under X-ray imaging through the arterial system to the vessels supplying the tumour. Once the feeding vessels are identified using contrast dye, an embolic agent, typically small particles, coils, or a liquid embolic material, is injected directly into those vessels. This physically occludes them, cutting off the blood supply to the tumour.
The procedure is typically performed 24 to 72 hours before surgery. During this window, the devascularised tumour begins to soften and its vascularity reduces substantially. When the surgeon then operates, the previously highly vascular tumour bleeds far less than it would have without embolisation, making the dissection safer and more controlled.
Embolisation is not always possible. When it is feasible, a Spine Vascular Surgeon in Dubai (Dr Sherief Elsayed – Leading Spine Surgeon in Dubai) works alongside the interventional radiology team to plan this pre-operative step. Its feasibility depends on the tumour’s location, the anatomy of its blood supply, and whether the feeding vessels can be safely occluded without compromising blood flow to critical structures such as the spinal cord or adjacent healthy bone. An experienced interventional radiologist assesses the angiographic anatomy before proceeding, and the decision to embolise is made jointly by the surgical and radiology teams.
Other Strategies for Managing Blood Loss in Spinal Tumour Surgery
Embolisation is the most powerful pre-operative tool, but it is part of a broader approach to haemorrhage management in complex spinal oncology cases.
Pre-operative blood preparation:
- Cross-matching blood for transfusion before surgery ensures that compatible blood is immediately available if needed
- Cell salvage devices collect blood that is lost during surgery, process it, and return it to the patient, reducing the need for donor blood transfusion
- Pre-operative autologous blood donation, where the patient donates their own blood weeks before surgery for use during the procedure, is used in selected cases
Surgical technique:
- Careful, anatomically precise dissection minimises the amount of tissue disturbed around the tumour
- Bipolar diathermy and topical haemostatic agents control bleeding from small vessels throughout the procedure
- Packing the surgical field and maintaining direct pressure allows the surgical team to manage active bleeding while maintaining surgical exposure
Anaesthetic management:
- Controlled hypotension, deliberately reducing blood pressure to a safe low level during the most vascular phases of the dissection, reduces the driving pressure behind bleeding
- Tranexamic acid, an antifibrinolytic medication given intravenously, reduces blood loss by preventing the breakdown of clots that form at bleeding points
- Careful fluid management and close monitoring of haemodynamic status throughout the procedure allows the anaesthetic team to respond quickly to significant blood loss
A Spine Tumour Surgeon in Dubai (Spine Tumour Treatment in Dubai) operating on vascular spinal metastases will apply all of these strategies in combination, with the specific combination tailored to the tumour type, location, and the patient’s overall condition.
What Types of Tumours Affect the Spine?
Understanding which tumours carry the highest haemorrhagic risk requires a brief overview of spinal tumour types.
Metastatic tumours are by far the most common. They originate elsewhere in the body and spread to the spine. The most common primary sources are lung, breast, prostate, kidney, thyroid, and bowel. Renal and thyroid metastases carry the highest vascular risk. Prostate metastases tend to be more sclerotic (bone-forming) and less vascular. Lung and breast metastases are intermediate.
Primary bone tumours of the spine are rare but include chordoma, giant cell tumour, osteosarcoma, and Ewing sarcoma. These require different treatment approaches from metastatic disease and are managed by specialist oncology teams.
Intradural tumours, arising within or adjacent to the spinal cord and its coverings, include meningioma, schwannoma, and ependymoma. These are often benign and highly curable with surgery, with blood loss typically less than metastatic vertebral tumours.
What Is the Goal of Surgery for Spinal Tumours?
The surgical goal depends on the tumour type, the extent of disease, the patient’s overall oncological situation, and the neurological status.
Indications for surgery in spinal tumours:
- Spinal cord or nerve root compression causing neurological deficit, which surgery can decompress to preserve or restore function
- Spinal instability from vertebral destruction, which surgery can stabilise to prevent deformity and further neurological injury
- Intractable pain from a tumour that has not responded to non-surgical measures
- Tissue biopsy for diagnosis when the primary source is unknown
- En bloc resection for selected primary bone tumours where cure is achievable
For metastatic disease, surgery is typically palliative rather than curative, aimed at preserving quality of life, maintaining neurological function, and providing spinal stability. A Spinal Reconstruction Surgeon in Dubai (Spinal Conditions – Diagnosis & Treatment in Dubai) will coordinate the multidisciplinary treatment plan for these cases. The decision to operate is made in the context of the patient’s overall prognosis. A Complex Spine Surgeon in Dubai (Dr Sherief Elsayed – Leading Spine Surgeon in Dubai) with experience in spinal oncology will coordinate this decision with the full multidisciplinary team., their functional status, and the availability of other treatment modalities including radiotherapy and systemic oncology treatment.
UAE-Specific Context
The UAE has one of the highest incidence rates of certain cancers in the region, and with an ageing population and a large expatriate community from diverse backgrounds, spinal metastases are a clinical reality that spine surgeons in Dubai manage regularly.
Access to interventional radiology for pre-operative embolisation, high-quality intraoperative imaging, and cell salvage technology is available at the major spinal centres where a UAE Spinal Oncology Surgeon (Dr Sherief Elsayed – Leading Spine Surgeon in Dubai) operates., high-quality intraoperative imaging, and cell salvage technology is available in the major surgical centres in Dubai and Abu Dhabi. The multidisciplinary approach, involving the spine surgeon, interventional radiologist, oncologist, and anaesthetist working together, is essential for achieving the best outcomes in these complex cases.
Expert Summary
The difference between losing 50 millilitres of blood during a discectomy and losing two litres during a tumour resection reflects a fundamental difference in the biology of what is being treated. Vascular spinal metastases, particularly from kidney and thyroid cancers, present one of the most technically demanding haemorrhagic challenges in elective surgery. Pre-operative embolisation, performed by an experienced interventional radiologist, is the most effective strategy for reducing this risk and making surgery safer.
Dr. Sherief Elsayed’s approach reflects the standard in specialist spinal oncology: thorough pre-operative planning, multidisciplinary preparation, and the use of every available tool to manage blood loss before it becomes a crisis rather than reacting to it during the procedure.
Table of Contents
Recent Articles

Why Leaning Backwards Makes Your Back Pain Worse and What It Means for Your Spine
Why Leaning Backwards Makes Your Back Pain Worse and What It Means for Your Spine Is facet joint pain the same as arthritis? Facet joint degeneration is essentially osteoarthritis of

Why an MRI Report Alone Is Not Enough to Decide on Spine Treatment in the UAE
Why an MRI Report Alone Is Not Enough to Decide on Spine Treatment in the UAE I have a disc protrusion on my MRI but no leg pain. Do I
General Anaesthesia vs Sedation, What Every Patient in Dubai Should Know Before Surgery
General Anaesthesia vs Sedation, What Every Patient in Dubai Should Know Before Surgery Will I feel anything during general anaesthesia? No. General anaesthesia eliminates consciousness, sensation, and awareness. You will
