Why an MRI Report Alone Is Not Enough to Decide on Spine Treatment in the UAE
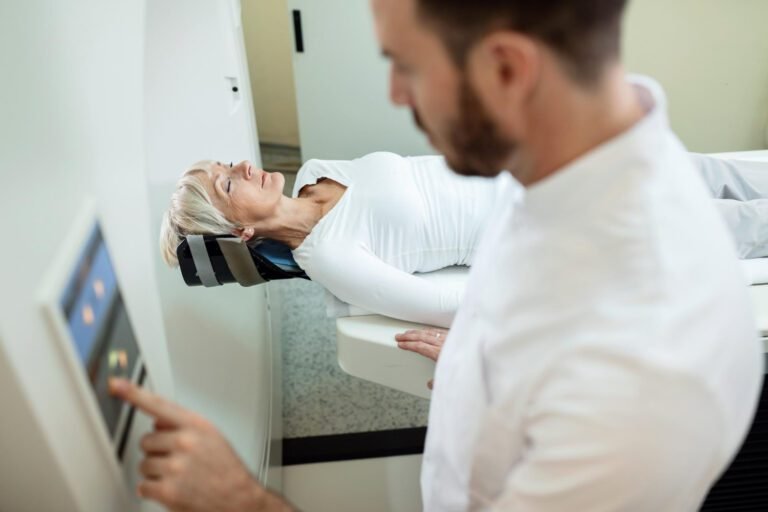
I have a disc protrusion on my MRI but no leg pain. Do I need treatment?
A disc protrusion without associated symptoms typically does not require specific treatment. Many people have disc protrusions on imaging and experience no symptoms at all. Monitoring and lifestyle advice are generally appropriate. If symptoms develop, reassessment is warranted.
My MRI shows canal stenosis. Does that mean I need surgery?
Canal stenosis on imaging requires clinical correlation. If it is associated with significant leg symptoms, progressive neurological deficit, or substantially impaired walking distance, surgery may be appropriate. If symptoms are mild or absent, conservative management is the appropriate starting point. The imaging finding alone does not determine the treatment.
What should I bring to my consultation besides the MRI report?
Bring the actual MRI images on a CD or USB drive, a list of your current symptoms including their duration and what makes them better or worse, a list of all medications you are taking, and a summary of any previous treatments you have tried for your back or leg symptoms.
Can Modic changes be treated?
Modic changes themselves do not reverse with any current treatment. However, the back pain associated with Type 1 Modic changes can be managed with targeted anti-inflammatory treatment, activity modification, and in selected cases, minimally invasive procedures. The changes are markers of inflammation at the disc-vertebra interface, and treatment is directed at managing the clinical symptoms they produce
Is it safe to wait before seeing a doctor about an MRI report?
For most findings, waiting for a routine appointment is appropriate. Patients in Dubai seeking a structured review of their MRI alongside a full clinical assessment should consult a Spine Assessment Doctor in Dubai (About Dr Sherief Elsayed – Consultant Spine Surgeon). However, if your symptoms include leg weakness that is worsening, loss of bladder or bowel control, or severe uncontrolled pain, do not wait. These require urgent assessment.
Why do radiologists report so many findings when many are not clinically significant?
Radiology reports are comprehensive by design. Interpreting what matters clinically is the role of a Diagnostic Spine Specialist in Dubai (Spinal Conditions – Diagnosis & Treatment in Dubai) with full examination skills. The radiologist’s role is to describe what is visible on the imaging, not to determine clinical significance in the context of a patient they have not examined. Clinical interpretation of the report, correlating findings with symptoms and examination, is the responsibility of the treating clinician.
Every day in Dubai, patients open a scan report on their phone, read a list of findings they do not fully understand, and immediately begin worrying about what it means for their health and whether they need surgery. Some of those patients arrive at consultations having already decided what treatment they need based on what they read. Others arrive terrified by language they cannot interpret. In almost every case, the scan alone is telling only part of the story.
Dr. Sherief Elsayed, Consultant Spine Surgeon in Dubai, addresses this directly through the lens of a real patient interaction: an MRI report of a lumbar spine shared with him on social media. His response reveals precisely why a scan report is not a diagnosis, and why the patient’s symptoms, not the imaging findings, must drive every treatment decision.
The Pre-Operative Context: Why Airway Safety Comes First
Before examining what an MRI report means, it is worth understanding one of the most important safety rules that governs any surgical treatment that might follow. Dr. Sherief Elsayed explains: “Some of the medications that we use can make you throw up. And if you throw up and you don’t have good control of your airway because you’re under anaesthesia, for example, you will aspirate. You will breathe that vomit in and you’ll end up with a nasty pneumonia, which can be life threatening.”
This is the clinical rationale behind pre-operative fasting, the instruction to avoid eating and drinking before surgery. Vomiting under anaesthesia, when the protective airway reflexes are suppressed, carries a risk of aspiration pneumonia that can be fatal. When emergency surgery cannot wait, a specific protective technique is used: “While we’re intubating you, while we’re putting the tube down to seal off the airway and protect it from any vomit, this assistant will press very hard down on here, which closes the oesophagus while the tube goes down.”
This manoeuvre, known as cricoid pressure, temporarily seals the oesophagus during intubation to prevent stomach contents from reaching the airway. It is the emergency safety net when fasting has not been possible. The routine safety measure is following fasting instructions precisely.
Understanding this context matters for any patient who may be moving toward surgical treatment following a scan: the preparation for surgery is itself part of the clinical pathway, and it begins before the operating table.
A Real MRI Report: What the Findings Actually Say
Dr. Sherief Elsayed describes reviewing an MRI scan report sent to him by a patient on social media: “Now I don’t know what symptoms they have, whether it’s back pain, leg symptoms, weakness, bladder or bowel dysfunction, but I see a lot of worrying findings in this report. Degenerative changes in the discs, there are Modic changes, which is inflammation within the bone itself. There is a disc protrusion causing canal stenosis, which would explain narrowing around the nerves and leg symptoms.”
This is a representative example of the kind of report that arrives in specialist inboxes regularly. It contains real and significant findings. But Dr. Sherief Elsayed’s first observation is not about the findings themselves. It is about what he does not know: the patient’s symptoms.
This ordering is deliberate and clinically important. The scan shows what the spine looks like. The symptoms reveal what the spine is doing to the patient. Only when both are known can treatment be properly directed.
What Do the Individual Findings Mean?
Degenerative Changes in the Discs
Disc degeneration refers to age-related and mechanical wear changes in the intervertebral discs. On MRI, degenerated discs appear darker on T2-weighted sequences (they have lost water content), reduced in height, and may show loss of the normal bright nucleus signal.
The critical clinical context is that disc degeneration is ubiquitous in adults. Studies of asymptomatic adults consistently show significant disc degeneration in a large proportion of people who have no back pain whatsoever. The presence of degeneration on imaging does not confirm it is the source of the patient’s pain. It is an anatomical finding, not a diagnosis.
Modic Changes
Modic changes are a more specific finding: changes in the vertebral end plates and adjacent bone marrow that represent an inflammatory response at the disc-vertebra interface. As Dr. Sherief Elsayed explains, they represent “inflammation within the bone itself.”
Type 1 Modic changes, which appear as increased fluid signal in the bone adjacent to the disc, represent active inflammation and are more clinically meaningful in the context of back pain. Type 2 changes represent a more chronic, stable phase. Type 1 Modic changes have the strongest association with discogenic pain, the deep aching back pain that arises from the disc and end plate complex rather than from nerve compression.
However, even Modic changes are not a definitive pain diagnosis. They indicate that the disc-vertebra interface is inflamed, but whether that inflammation is the primary driver of a patient’s symptoms requires clinical correlation.
Disc Protrusion Causing Canal Stenosis
This finding is the most clinically significant in the report. A disc protrusion is a focal extension of disc material beyond the normal disc margins. When it protrudes into the spinal canal, it reduces the space available for the nerve roots. Canal stenosis means narrowing of that space. When the narrowing is sufficient to compress a nerve root, symptoms develop.
As Dr. Sherief Elsayed notes, this finding “would explain narrowing around the nerves and leg symptoms.” The key word is “would.” The finding has the potential to explain leg symptoms. Whether it is actually causing leg symptoms in this specific patient requires knowing what the patient actually experiences.
A disc protrusion causing canal stenosis in a patient with severe sciatica, progressive leg weakness, and reduced reflexes is a finding requiring active clinical management. The same finding in a patient with mild intermittent back pain and no leg symptoms may warrant only monitoring and conservative management. The scan is identical. The clinical situation is entirely different.
What the Patient Actually Needs to Do
Dr. Sherief Elsayed’s advice is specific and practical: “What this patient needs to do is get the images of his MRI scan, see his local doctor who will ask him a series of questions and then depending on his symptoms, you’ll either guide him towards non-operative measures or if he has a lot of leg symptoms, for example, he may be a candidate for surgical intervention.”
This guidance contains several layers worth unpacking.
Get the images, not just the report. A written radiology report is a summary. The actual MRI images carry far more information and allow the treating clinician to assess the degree of compression, the specific anatomy of the neural structures involved, and the relationship between the findings and the patient’s body that the report cannot fully convey.
See a doctor who will take a history. The sequence of clinical reasoning is symptoms first, imaging second. A clinician who looks at the scan before asking about the patient’s experience of their problem is working in the wrong order. The history and examination establish the clinical picture; imaging confirms or clarifies it.
Treatment follows symptoms, not scan findings. This is the core principle. Non-operative measures are appropriate when symptoms are manageable, when there is no significant neurological deficit, and when the patient has not yet had an adequate trial of conservative management. Surgical candidacy requires a combination of clinical severity, failure of appropriate non-operative care, and imaging that confirms a surgically treatable structural problem. The scan alone determines none of this.
A Nerve Compression Specialist in Dubai (Nerve Compression Treatment – Dubai Spine Specialist) will always assess imaging in the full context of the clinical presentation, mapping symptoms against findings to determine what is clinically significant and what requires treatment.
The Danger of Treating the Scan Rather Than the Patient
The consequences of treating imaging findings rather than clinical symptoms are well documented and represent one of the most significant sources of avoidable harm in spine care.
Over-investigation: Patients with incidental findings are referred for further imaging, generating anxiety and additional cost without changing the management of their actual clinical problem.
Inappropriate surgery: Operating on a finding that is not causing the patient’s symptoms produces no improvement in those symptoms. The patient’s pain continues, attributable to a cause that was never identified because the scan dominated the clinical assessment.
Nocebo effect: Patients who are told they have “degenerative changes” or “stenosis” on their scan may develop worsening symptoms because of anxiety about those findings, even when the findings would otherwise have remained asymptomatic. The language used around imaging findings has real clinical consequences.
Missed diagnosis: When clinical attention focuses entirely on the scan, other causes of the patient’s symptoms may be overlooked. A patient with back pain and a degenerated disc on MRI may actually have pain from facet joints, sacroiliac joints, or a structure not well visualised on that imaging study.
Red Flags That Require Urgent Action Regardless of MRI Findings
While most MRI findings can be assessed in a routine outpatient setting, certain clinical scenarios require urgent or emergency review. These are defined by symptoms, not by scan findings.
Seek immediate assessment if you experience:
- Loss of bladder or bowel control alongside back or leg pain
- Numbness in the inner thighs, groin, or saddle area
- Rapidly progressive weakness in both legs
- Severe pain following significant trauma
These presentations may indicate cauda equina syndrome or acute spinal cord compression, both of which require emergency surgical assessment. The imaging may be severe or the imaging may be less dramatic than the clinical picture suggests, but the urgency is defined by the symptoms, not the scan.
Expert Summary
An MRI report is the beginning of a clinical assessment, not the conclusion of one. Degenerative changes, Modic changes, and disc protrusions causing canal stenosis are all significant findings. They are also findings that exist in people with no symptoms, mild symptoms, and severe symptoms alike. What determines the clinical meaning of those findings, and what treatment if any is appropriate, is always the patient’s symptom picture, examined alongside the imaging.
Dr. Sherief Elsayed’s response to the patient who shared their MRI on social media is the same response he gives in clinic every day: get the images, see someone who will ask you the right questions, and let the symptoms, not the scan, guide the treatment decision. To discuss your MRI findings in the context of your actual symptoms, consulting a UAE Spine Surgeon (Dr Sherief Elsayed – Leading Spine Surgeon in Dubai) is the most direct way to understand what those findings actually mean for you.
Table of Contents
Recent Articles

Why Leaning Backwards Makes Your Back Pain Worse and What It Means for Your Spine
Why Leaning Backwards Makes Your Back Pain Worse and What It Means for Your Spine Is facet joint pain the same as arthritis? Facet joint degeneration is essentially osteoarthritis of

Why an MRI Report Alone Is Not Enough to Decide on Spine Treatment in the UAE
Why an MRI Report Alone Is Not Enough to Decide on Spine Treatment in the UAE I have a disc protrusion on my MRI but no leg pain. Do I
General Anaesthesia vs Sedation, What Every Patient in Dubai Should Know Before Surgery
General Anaesthesia vs Sedation, What Every Patient in Dubai Should Know Before Surgery Will I feel anything during general anaesthesia? No. General anaesthesia eliminates consciousness, sensation, and awareness. You will
