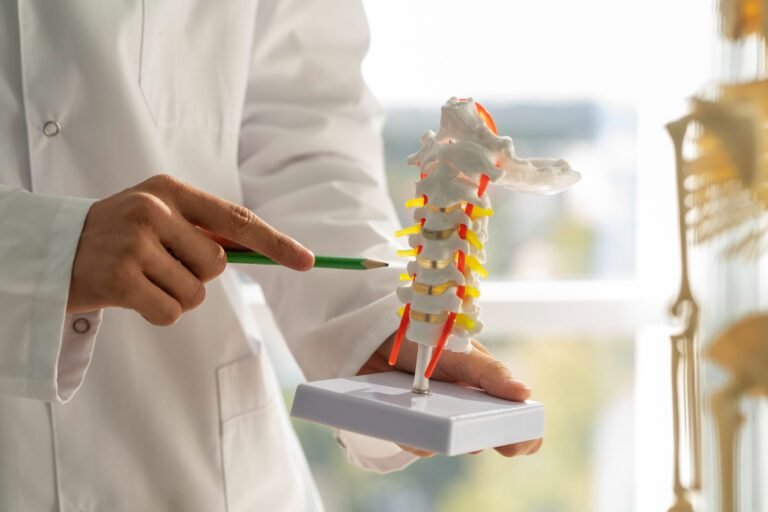
Should You Get a Spinal Fusion for Lower Back Pain? A Dubai Surgeon Tells the Truth
Is spinal fusion a permanent operation?
Yes. Once the vertebrae have fused, the movement between them is permanently eliminated. The metalwork used to achieve the fusion typically remains in place for life unless it causes specific problems. The decision should be treated as irreversible.
How long does recovery from spinal fusion take?
Recovery depends on the number of levels fused, the approach used, and the patient’s overall health. Most patients are mobile within a day or two of surgery. Return to light work typically takes four to eight weeks. Full fusion and return to heavy physical activity takes six to twelve months.
Does fusion always spread to adjacent levels?
Adjacent segment degeneration is a recognised long-term consequence of lumbar fusion, occurring in a proportion of patients over years to decades. The risk is higher with longer fusions and at certain spinal levels. It does not always cause symptoms, and not all adjacent segment changes require further surgery.
Can I have physiotherapy instead of fusion?
For many patients with back pain, including those who have been told they need fusion, a structured course of physiotherapy, pain management, and rehabilitation has not yet been adequately tried. In the absence of significant neurological compromise or clear structural instability, physiotherapy-led rehabilitation should always precede any discussion of elective fusion.
Will fusion stop my back pain completely?
Not necessarily, and this is one of the central challenges of fusion for back pain. Even technically successful fusion with good bone healing does not guarantee pain relief. Patient selection is the most important predictor of outcome. Patients with clear structural targets, minimal psychological contributors to pain, and good baseline function tend to have the best results.
Should I get a second opinion before agreeing to fusion?
For any elective surgical procedure, and particularly for an irreversible one such as spinal fusion, seeking a second opinion is entirely appropriate. A Spinal Stability Surgeon in Dubai (Spinal Conditions – Diagnosis & Treatment in Dubai) can provide an independent assessment of whether fusion is genuinely indicated. and should be welcomed by any surgeon confident in their recommendation.
Spinal fusion is one of the most performed and most debated operations in spinal surgery. In some parts of the world, patients with chronic lower back pain are offered fusion almost as a routine response. In others, including the United Kingdom where Dr. Sherief Elsayed trained, the threshold is considerably more cautious. Understanding the difference matters enormously, because fusion is a major operation with permanent consequences that cannot be reversed.
Dr. Sherief Elsayed, Consultant Spine Surgeon in Dubai, is direct on this subject. His position is grounded in clinical evidence and reflects the standard he was trained to uphold.
What Is Spinal Fusion?
Spinal fusion is a surgical procedure that permanently joins two or more vertebrae together, eliminating movement between them. It is achieved by placing bone graft material between the vertebrae, often supplemented by metal implants including screws, rods, and cages, which hold the bones in the correct position while the graft heals and the segment fuses into a single solid structure.
Once fused, that segment of the spine no longer moves independently. The aim is to eliminate the painful movement at that level and, depending on the indication, to restore alignment, decompress nerves, or stabilise an unstable segment.
Fusion is highly effective for specific, well-defined indications. It is significantly less effective when applied to the wrong problem.
What Is the Difference Between Fusion for Back Pain and Fusion for Back Pain With Leg Symptoms?
This distinction is central to Dr. Sherief Elsayed’s clinical position, and he states it plainly: “I’m talking about fusion for back pain. Fusion for back pain with leg symptoms, different story.”
Fusion for pure lower back pain means operating to address axial pain, the deep aching pain localised to the lower back without significant radiating symptoms. The evidence base for this indication is contested and has been for decades. The assumption is that the painful motion at a degenerated disc level can be eliminated by fusing it. In practice, identifying which disc is truly generating the pain, and predicting which patients will respond well to fusion, has proven consistently difficult.
Fusion for back pain with leg symptoms addresses a structural problem, typically nerve root compression from disc herniation, spinal stenosis, or spondylolisthesis, where the spinal segment is also unstable or deformed. Here the surgical target is clear, the nerve compression can be confirmed on imaging and examination, and the fusion provides the stability needed to decompress the nerve effectively and prevent recurrence. The evidence base for this indication is considerably stronger.
What Is the Standard in the United Kingdom?
Dr. Sherief Elsayed trained in the NHS and is clear about what that environment taught him: “In the United Kingdom where I was trained, you do not have a low back fusion for back pain outside of a clinical trial.”
This is not simply a cost-containment policy. It reflects the conclusions of a substantial body of clinical evidence, including large randomised controlled trials that have compared fusion to intensive non-surgical rehabilitation for non-specific chronic lower back pain. Several of these studies have found that the outcomes between the two groups are not significantly different at long-term follow-up.
NICE guidance in the UK does not recommend spinal fusion as a treatment for non-specific low back pain. This position is supported by systematic reviews consistently showing that outcomes for fusion in this indication are unpredictable and that a meaningful proportion of patients experience no improvement, or even deterioration.
Why Is Fusion Offered More Readily in Some Countries?
Dr. Sherief Elsayed acknowledges this directly: “In other countries, I won’t name which, you will be offered a fusion almost immediately.”
Several factors contribute to this variation in practice. Healthcare system incentives, reimbursement structures, and patient demand all play a role. In privately funded healthcare settings, there can be a commercial driver toward more surgical intervention. Patient expectations also vary, with some patients arriving having already decided they need surgery and seeking a surgeon who will provide it.
This does not mean that surgeons offering fusion in these settings are acting incorrectly in every case. It means that the threshold for surgery varies and that patients seeking care across different healthcare systems need to understand that variation when interpreting advice they receive.
A Spine Surgeon in Dubai (Spinal Conditions – Diagnosis & Treatment in Dubai) who follows evidence-based practice will apply a consistent threshold regardless of the setting, using the same clinical criteria that would be applied in a well-resourced specialist centre anywhere in the world.
Why Fusion for Pure Back Pain Is a High-Stakes Decision
Dr. Sherief Elsayed’s caution about fusion for back pain reflects two specific concerns that he articulates clearly: “That’s very difficult to determine who’s going to respond well and it can leave some patients worse off. It’s something you can’t undo.”
Difficulty predicting responders: Chronic lower back pain is a complex condition with structural, neurological, psychological, and social components. A Spine Pain Doctor in Dubai (Spinal Conditions – Diagnosis & Treatment in Dubai) can determine whether your pain has a structural surgical target or requires a different pathway. Even when imaging shows degeneration at a specific level, that degeneration may not be the primary pain generator. Fusion eliminates movement at the targeted level but cannot address the other components of chronic pain. Patients who have significant central sensitisation, psychological contributors to pain, or who have had prolonged pain with significant functional decline may not respond to a structural fix regardless of its technical success.
The permanence of the decision: Fusion cannot be reversed. If the outcome is poor, the options are limited. Revision surgery at the same level is technically demanding and often carries worse outcomes than the primary procedure. Adjacent segment degeneration, where the disc above or below the fusion accelerates its own deterioration. A Revision Spine Surgeon in Dubai (Dr Sherief Elsayed – Leading Spine Surgeon in Dubai) has the specialist experience to manage these complex cases. due to increased mechanical stress, is a well-documented long-term consequence that may require further surgery years later.
These two factors together mean that the decision to fuse for back pain without leg symptoms demands a very high level of certainty that is rarely achievable with current diagnostic tools.
When Is Fusion the Right Decision?
Despite the caution around fusion for pure back pain, there are well-established indications where fusion is clearly appropriate and produces excellent outcomes.
Strong indications for lumbar fusion include:
- Spondylolisthesis with nerve compression or instability causing significant symptoms that have failed conservative management
- Spinal stenosis requiring decompression at a level that is also unstable, where decompression alone would risk progressive instability
- Revision surgery following prior decompression that has created instability
- Spinal fracture with instability
- Spinal tumour requiring structural reconstruction
- Adult degenerative scoliosis causing significant pain and functional decline
- Discogenic pain with a clearly positive provocation discogram in a carefully selected patient, though this indication remains more controversial
In each of these situations, the surgical target is structural and well-defined, the relationship between the pathology and the symptoms is clear, and the evidence for a good outcome with fusion is substantially stronger than for pure back pain.
What Should Patients in Dubai Ask Before Agreeing to Fusion?
Any patient being offered lumbar fusion for lower back pain without significant leg symptoms should ask the following questions before consenting.
Questions worth asking:
- What specifically is causing my pain and how has that been confirmed?
- What is the evidence that fusion will address that specific cause?
- What non-surgical options have I not yet tried, and have they been given a proper trial?
- What are the risks specific to my anatomy and health?
- What does the long-term evidence show for fusion at my level for my indication?
- What happens if the fusion does not relieve my pain?
A surgeon who welcomes these questions and provides clear, evidence-based answers is one whose recommendation can be trusted. A surgeon who discourages them is one worth seeking a second opinion from. Consulting a Back Pain Doctor in Dubai (Back Pain Treatment in Dubai – Rapid Relief & Rehabilitation) for an independent assessment before committing to any irreversible procedure is always appropriate.
UAE-Specific Context
In the UAE’s private healthcare environment, patients frequently have rapid access to specialist consultations, advanced imaging, and surgical procedures. This accessibility is a genuine advantage in many clinical situations. In the context of elective lumbar fusion for back pain, it means that the decision to operate can sometimes be reached more quickly than the clinical evidence warrants.
Patients in Dubai should be aware that the standard of care for fusion in non-specific back pain, as defined by the evidence base, does not support routine operative intervention. A recommendation for fusion should be accompanied by a clear explanation of why conservative management is no longer appropriate, what specific structural problem the fusion is targeting, and what the realistic outcomes are for that indication in that patient.
Expert Summary
Spinal fusion is a powerful and effective operation for the right indication. For lower back pain without leg symptoms, without clear instability, and without a well-defined structural target, the evidence does not support routine fusion and the outcomes are unpredictable. For back pain with leg symptoms arising from a structural problem that requires surgical stabilisation, fusion can be transformative.
Dr. Sherief Elsayed’s position is not anti-surgical. It is pro-precision. The operation should match the problem, the problem should be confirmed beyond reasonable doubt, and the permanence of the decision should be weighed carefully before any patient consents to a fusion for back pain alone.
Table of Contents
Recent Articles
Should You Get a Spinal Fusion for Lower Back Pain? A Dubai Surgeon Tells the Truth
Should You Get a Spinal Fusion for Lower Back Pain? A Dubai Surgeon Tells the Truth Is spinal fusion a permanent operation? Yes. Once the vertebrae have fused, the movement

When Does Scoliosis Actually Need Surgery? A UAE Spine Surgeon Explains the Threshold
When Does Scoliosis Actually Need Surgery? A UAE Spine Surgeon Explains the Threshold At what curve size does scoliosis definitely need surgery? The surgical threshold is generally 45 to 50

Not All Sciatica Comes From a Slipped Disc: A Dubai Spine Surgeon Explains Why
Not All Sciatica Comes From a Slipped Disc: A Dubai Spine Surgeon Explains Why Can spondylolisthesis be present without causing any symptoms? Yes. Many cases are discovered incidentally on imaging
