General Anaesthesia vs Sedation, What Every Patient in Dubai Should Know Before Surgery
Will I feel anything during general anaesthesia?
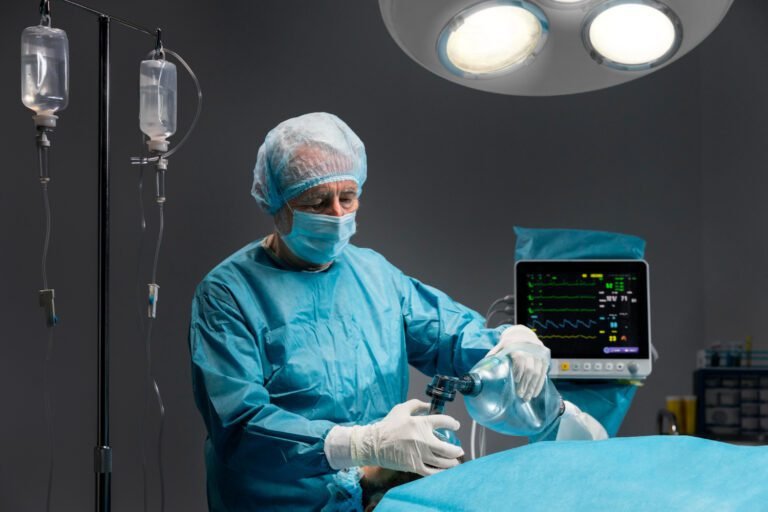
No. General anaesthesia eliminates consciousness, sensation, and awareness. You will have no memory of the procedure and will not experience pain or discomfort during it. The transition into and out of anaesthesia is managed carefully by the anaesthetic team.
Can I choose to have sedation instead of general anaesthesia for spine surgery?
The anaesthetic technique is determined by clinical requirements, not purely by patient preference. Major spinal procedures require general anaesthesia for patient safety and to allow the procedure to be performed correctly. Sedation is appropriate for minor interventional procedures but not for major surgery.
Why does my throat hurt after surgery?
A sore throat after general anaesthesia is caused by the endotracheal tube and typically resolves within one to two days. It is a minor and expected consequence of airway management during general anaesthesia.
What is the risk of general anaesthesia?
General anaesthesia is very safe in healthy patients when administered by trained anaesthetists with appropriate monitoring. The risk of serious complications including death from anaesthesia alone is extremely low in elective surgical settings. Risks increase with age, obesity, pre-existing medical conditions, and emergency surgery.
Will I feel sick after the operation?
Post-operative nausea and vomiting affects between 20 and 40 percent of patients following general anaesthesia without prophylaxis. Modern anti-emetic protocols significantly reduce this risk. Patients with a history of post-operative nausea should inform the anaesthetic team. A Spine Pre-Op Specialist in Dubai (Spinal Conditions – Diagnosis & Treatment in Dubai) will ensure this information is passed to the anaesthetic team during your pre-operative assessment., as specific preventive measures can be applied.
Can I eat or drink before a procedure under sedation?
The fasting requirements for sedation are generally the same as for general anaesthesia. Even under sedation, the risk of aspiration if vomiting occurs means the stomach should be empty before the procedure. Always follow the specific fasting instructions provided by your surgical team.
The prospect of surgery raises many questions, and one of the most common is about anaesthesia. Patients often use the phrase “being put to sleep” to describe the process, but that single phrase covers a range of very different clinical states. Local anaesthesia, sedation, and general anaesthesia are not variations on the same thing. They are fundamentally different techniques with different mechanisms, different applications, and different implications for what the patient experiences and what the surgical team can safely do.
Dr. Sherief Elsayed, Consultant Spine Surgeon in Dubai, explains the distinction clearly and practically, including the specific reasons why certain spine procedures require not just general anaesthesia but the addition of paralysing agents as well.
What Is Local Anaesthesia?
Local anaesthesia is the most limited form of anaesthetic intervention. It involves injecting an anaesthetic agent directly into or around the tissue that needs to be numbed, producing a loss of sensation in that localised area without affecting consciousness or any other part of the body.
Dr. Sherief Elsayed uses a familiar example: “Local anaesthesia is where we just inject. So I have a little skin lump here, I want it removed. So I’ll inject some local anaesthetic, make my incision, take out the skin.”
The patient is fully awake and alert throughout. The anaesthetic agent blocks the transmission of pain signals from the nerve endings in the injected area, but the patient remains conscious, breathing independently, and in complete control of their own airway.
Local anaesthesia is appropriate for superficial procedures such as skin lesion removal, minor wound repair, and certain outpatient diagnostic procedures. It is not appropriate for procedures that require access to deeper structures, that involve significant pain or discomfort beyond what can be blocked locally, or that require the patient to remain completely still for an extended period.
In spine care, local anaesthesia is used for minimally invasive procedures such as diagnostic facet joint injections, nerve root blocks, and radiofrequency denervation, where a precise volume of anaesthetic is delivered to a specific target under imaging guidance.
What Is Sedation?
Sedation occupies the middle ground between local anaesthesia and general anaesthesia. It involves administering medication intravenously that produces a state of reduced consciousness ranging from mild relaxation to deep sleep, depending on the dose and the agent used.
Dr. Sherief Elsayed describes it precisely: “Sedation means that we give you a special medicine intravenously whilst you’re being oxygenated, and that puts you to sleep.”
The key characteristic of sedation is that, unlike general anaesthesia, the patient retains their protective airway reflexes and breathes independently. They do not have a tube in their airway. They can be roused by stimulation in lighter levels of sedation, though in deeper procedural sedation they may be unresponsive to verbal stimuli.
Levels of sedation:
- Minimal sedation (anxiolysis): the patient is relaxed but fully awake and responsive
- Moderate sedation: the patient is drowsy and may fall asleep but can be easily awakened and responds to verbal commands
- Deep sedation: the patient is difficult to rouse and may not respond reliably to verbal stimuli, though protective airway reflexes are usually maintained
- General anaesthesia: the patient is completely unconscious, airway reflexes are suppressed, and the airway must be managed externally
The boundary between deep sedation and general anaesthesia is not always clinically sharp, which is why sedation for procedures is always managed by trained anaesthetic personnel with appropriate monitoring and the ability to manage the airway if needed.
In spine care, sedation is commonly used for procedures such as epidural injections, discography, and other interventional pain management procedures where the patient needs to be comfortable but may also need to provide feedback on symptoms during the procedure.
What Is General Anaesthesia?
General anaesthesia is a controlled state of unconsciousness in which the patient has no awareness, no sensation, and no ability to protect their own airway. It requires active management of the airway throughout the procedure.
Dr. Sherief Elsayed explains the defining feature: “General anaesthesia means that there’s a tube going down and that is ventilating your lungs with oxygen. There’s a filter which absorbs carbon dioxide and that makes sure you’re deep, deep asleep.”
The tube Dr. Sherief Elsayed refers to is an endotracheal tube, which is passed through the mouth, through the vocal cords, and into the trachea (windpipe). Once in place and its cuff inflated, it seals the airway, preventing aspiration of stomach contents and allowing the anaesthetic machine to control the patient’s ventilation completely. Oxygen is delivered, carbon dioxide is removed, and the concentration of inhaled anaesthetic agent is precisely controlled to maintain the required depth of anaesthesia throughout the procedure.
Why general anaesthesia is required for major spine surgery:
Major spinal procedures including discectomy, decompression, fusion, and scoliosis correction cannot be safely performed under sedation. The patient must be completely still for extended periods, often in positions that are not possible for a conscious patient, and the depth and duration of anaesthesia required cannot be reliably achieved without a secured airway and controlled ventilation.
The prone position commonly used for posterior spinal surgery, in which the patient lies face down for the duration of the procedure, is only safely possible under general anaesthesia with a secured airway.
Why Are Paralysing Agents Used in Spine Surgery?
Dr. Sherief Elsayed adds an important detail that is rarely discussed with patients: “In addition to general anaesthesia, we also use paralyzing agents. That’s very, very helpful if, for example, I’m doing a lot of muscle peeling. It makes it much easier for me to pull that muscle away.”
Neuromuscular blocking agents, commonly called paralysing agents or muscle relaxants, temporarily block the transmission of signals from motor nerves to muscles, causing complete muscle paralysis throughout the body. The patient is already unconscious and has no awareness of this; the paralysis is relevant only to the surgical and anaesthetic teams.
Why paralysis is useful in spine surgery:
Posterior spinal approaches require the paraspinal muscles, which run in strong columns on either side of the spine, to be retracted away from the bone to provide surgical access. In an unparalysed patient under general anaesthesia, these muscles retain residual tone that makes retraction more difficult and may require greater force to achieve adequate exposure. Paralysis eliminates this muscle tone, making the dissection and retraction smoother, reducing the force required, and potentially reducing the trauma to the muscles during exposure.
The airway implication:
Because paralysing agents also paralyse the respiratory muscles, a patient receiving these agents is entirely dependent on mechanical ventilation. This is why the endotracheal tube and ventilator are not optional when paralysing agents are used. The combination of general anaesthesia and neuromuscular blockade represents the deepest and most controlled form of anaesthetic management, and it requires continuous monitoring of the airway, ventilation, and neuromuscular function throughout.
Monitoring During General Anaesthesia
General anaesthesia for spine surgery involves continuous monitoring of multiple physiological parameters. This level of care is standard at all major spinal surgical centres where a Specialist Spine Surgeon in Dubai (Dr Sherief Elsayed – Leading Spine Surgeon in Dubai) operates. throughout the procedure.
Standard monitoring includes:
- Pulse oximetry, measuring blood oxygen saturation continuously
- Capnography, measuring exhaled carbon dioxide to confirm correct tube placement and adequate ventilation
- Electrocardiography, monitoring heart rhythm and rate
- Blood pressure measurement at regular intervals or continuously via an arterial line in complex cases
- Temperature monitoring, as prolonged surgery under anaesthesia can cause hypothermia
- Neuromuscular monitoring, tracking the degree of muscle blockade to ensure adequate paralysis when needed and complete reversal before the patient is woken
For scoliosis correction and other procedures where neurological function is at risk, neuromonitoring of the spinal cord using evoked potentials is added to this standard monitoring package.
What Happens When Anaesthesia Ends?
The process of waking from general anaesthesia is as carefully managed as the induction and maintenance. Anaesthetic agents are reduced, paralysing agents are reversed pharmacologically, and the patient’s breathing is assessed before the endotracheal tube is removed. Patients are transferred to a recovery area where they are monitored as they regain full consciousness and protective airway reflexes.
Post-operative nausea and vomiting is a common side effect of general anaesthesia, managed with anti-emetic medications given during and after the procedure. Shivering, sore throat from the endotracheal tube, and temporary confusion are also common and transient.
The pre-operative fasting requirement, typically nothing to eat for six hours and nothing to drink except clear fluids for two hours before surgery, exists precisely to reduce the risk of aspiration if vomiting occurs under anaesthesia. Understanding why this rule exists, and why it must be followed strictly, is covered in detail elsewhere in this blog.
Choosing the Right Anaesthetic Approach for Your Procedure
The anaesthetic technique for any given procedure is chosen by the anaesthetic team. Patients should feel free to ask their Orthopaedic Spine Surgeon in Dubai (Spinal Conditions – Diagnosis & Treatment in Dubai) any questions about planned anaesthesia at the consent consultation. based on the nature of the procedure, the expected duration, the required patient position, the depth of anaesthesia needed, and the patient’s individual medical history.
For spine patients in Dubai, this decision is made at the pre-operative anaesthetic assessment. Patients with specific concerns about anaesthesia, including previous adverse reactions or particular anxiety about any aspect of the process, should raise these with both the anaesthetic team and their UAE Back Pain Surgeon (Back Pain Treatment in Dubai – Rapid Relief & Rehabilitation) at the pre-operative consultation., including previous adverse reactions, family history of anaesthetic problems, or particular anxiety about any aspect of the process, should raise these at that assessment. The anaesthetic team will accommodate reasonable concerns and provide specific information about what to expect.
A Spine Consultant in Dubai (Contact Dr Sherief Elsayed – Book an Appointment) will ensure that the pre-operative assessment covers all the relevant medical, anaesthetic, and surgical considerations before your procedure date.
Expert Summary
Local anaesthesia numbs a small area without affecting consciousness. Sedation reduces awareness while preserving independent breathing and airway reflexes. General anaesthesia renders the patient completely unconscious with a secured, managed airway. Paralysing agents are added in procedures where complete muscle relaxation significantly improves surgical access and safety.
Each technique has its appropriate application, and the choice is made by the anaesthetic team based on clinical requirements rather than patient preference alone. For major spine surgery, general anaesthesia with neuromuscular blockade is the standard and most appropriate approach. Understanding why each element is part of the process makes the experience less frightening and more collaborative.
Table of Contents
Recent Articles

Why Leaning Backwards Makes Your Back Pain Worse and What It Means for Your Spine
Why Leaning Backwards Makes Your Back Pain Worse and What It Means for Your Spine Is facet joint pain the same as arthritis? Facet joint degeneration is essentially osteoarthritis of

Why an MRI Report Alone Is Not Enough to Decide on Spine Treatment in the UAE
Why an MRI Report Alone Is Not Enough to Decide on Spine Treatment in the UAE I have a disc protrusion on my MRI but no leg pain. Do I
General Anaesthesia vs Sedation, What Every Patient in Dubai Should Know Before Surgery
General Anaesthesia vs Sedation, What Every Patient in Dubai Should Know Before Surgery Will I feel anything during general anaesthesia? No. General anaesthesia eliminates consciousness, sensation, and awareness. You will
